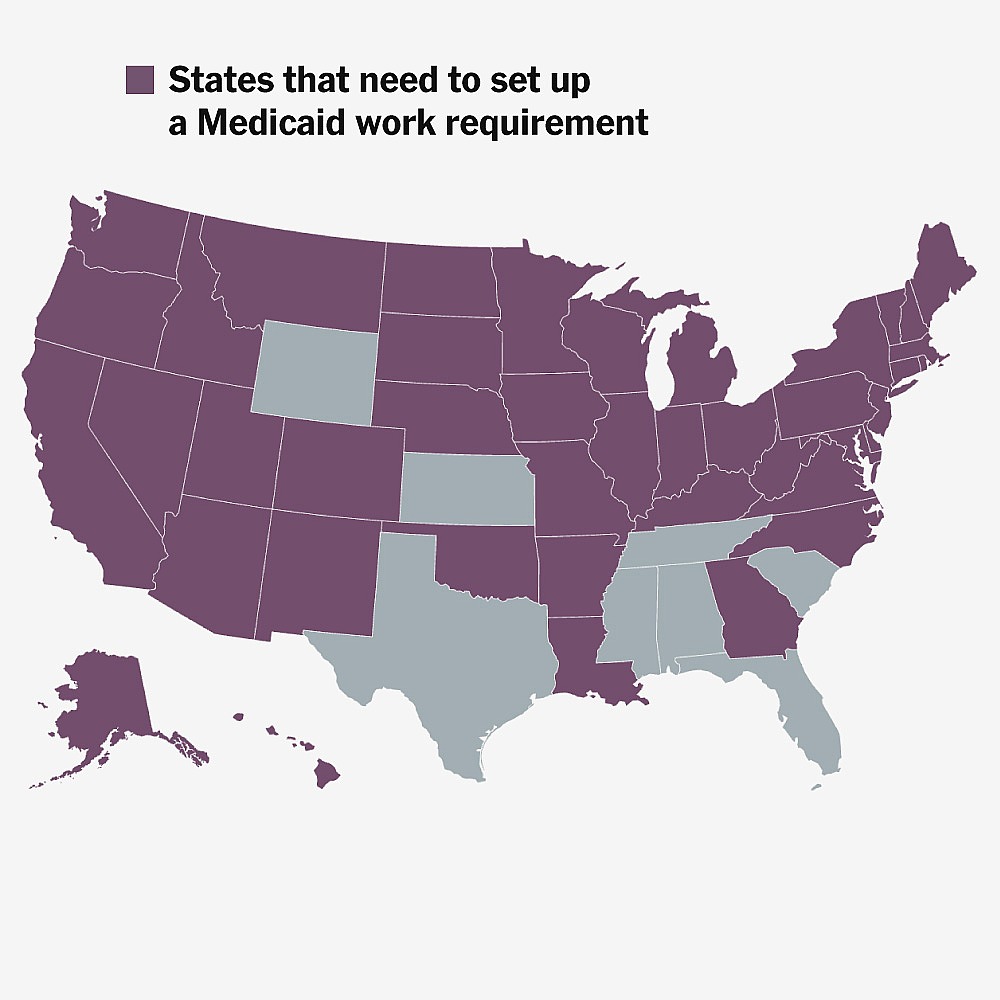
How Medicaid’s New Work Requirement Will Work
In a significant shift affecting low-income Americans, new enrollment challenges are set to emerge as states navigate the complexities of healthcare access. With the expiration of the COVID-19 public health emergency, many states are transitioning from temporary measures that allowed for streamlined Medicaid enrollment to more stringent processes. This change is particularly concerning for millions of Americans who rely on these programs for essential health services. States are now tasked with building new bureaucratic frameworks to manage the influx of renewals and new applications, a process that could lead to increased confusion and potential disenrollment for vulnerable populations.
For context, during the pandemic, many states implemented policies that prevented Medicaid disenrollment, allowing individuals to maintain coverage without the usual verification processes. However, as these protections wane, states are required to reassess eligibility based on income and other criteria, which could result in many individuals losing their coverage. For example, a recent report highlighted that nearly 15 million people could be at risk of losing Medicaid as states begin to redetermine eligibility. The new bureaucratic processes will require states to hire additional staff, upgrade technology, and develop outreach programs to ensure that those who are eligible can successfully navigate the system. This transition not only poses logistical challenges but also raises concerns about the potential for increased health disparities among low-income populations.
As states grapple with these new responsibilities, advocates warn that the lack of adequate resources and infrastructure could lead to significant gaps in coverage. Many low-income Americans already face barriers such as limited access to information and support, which could be exacerbated by the new enrollment complexities. The implications of these changes are profound, as losing access to Medicaid can lead to delayed care, increased medical debt, and poorer health outcomes. Policymakers and healthcare advocates are calling for swift action to ensure that these vulnerable populations are not left behind during this critical transition, emphasizing the need for comprehensive outreach and support systems to facilitate a smoother enrollment process. As the landscape of healthcare access evolves, the focus must remain on protecting the most vulnerable and ensuring that essential health services remain accessible to all.
Poor Americans will face new challenges to enroll, and states will have to build new bureaucracies.