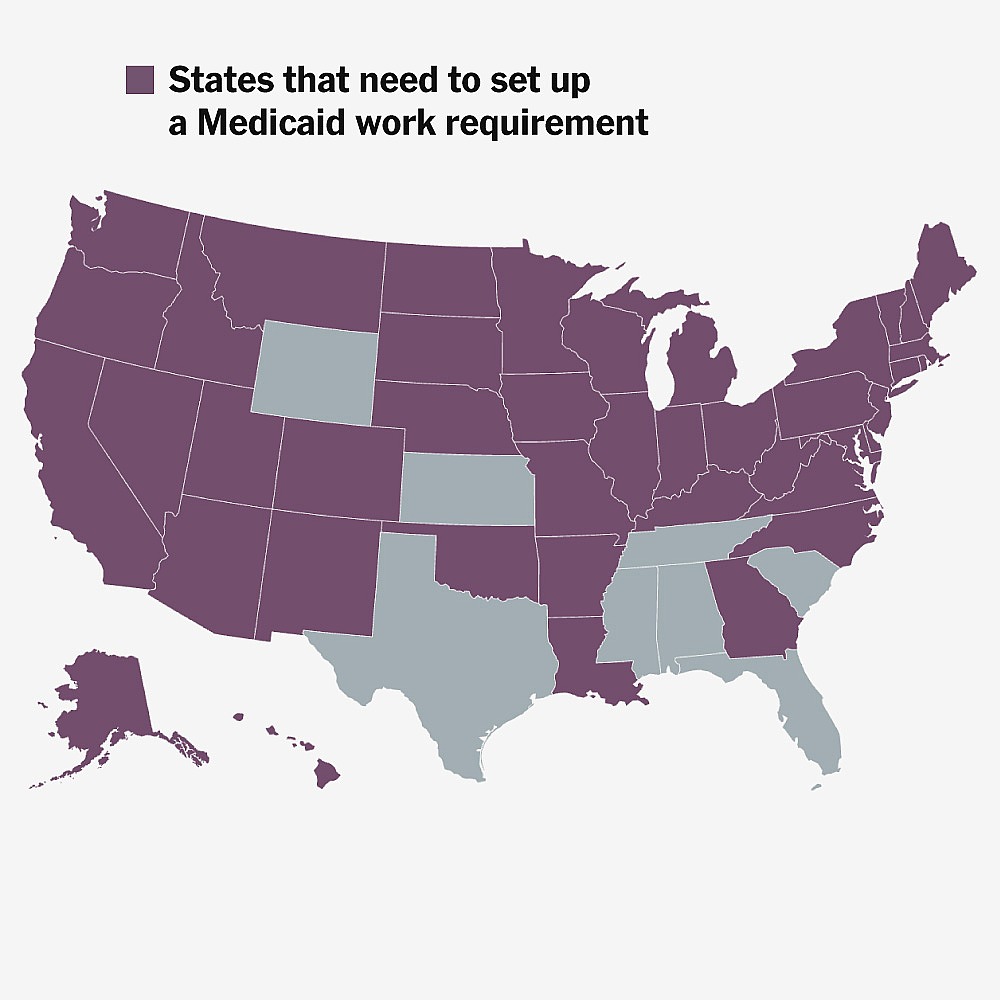
How Medicaid’s New Work Requirement Will Work
In a significant shift for low-income Americans seeking health coverage, recent changes to Medicaid enrollment processes are set to create additional hurdles for millions. Following the end of the COVID-19 public health emergency, states are required to reassess the eligibility of Medicaid recipients, a move that could result in many losing their coverage. The transition from the relaxed enrollment policies implemented during the pandemic back to more stringent eligibility checks raises concerns about the potential for increased uninsured rates among vulnerable populations. With an estimated 15 million people at risk of losing their Medicaid benefits, the implications of this policy shift are profound, particularly in states that have historically struggled with healthcare access.
To navigate these changes, states must establish new bureaucratic systems to manage the influx of re-enrollment applications and eligibility determinations. This includes hiring additional staff, implementing updated technology systems, and developing outreach programs to ensure that individuals are aware of their rights and options. For instance, states like Texas and Florida, which have large populations of Medicaid recipients, will need to ramp up their efforts to handle the anticipated surge in administrative work. Moreover, many low-income individuals may face challenges in understanding the new enrollment requirements, particularly those who lack access to reliable internet or have language barriers. This situation is compounded by the fact that many recipients may not be aware that they need to reapply, leading to potential lapses in coverage.
The stakes are high, as losing Medicaid coverage not only impacts individuals’ access to essential healthcare services but also places additional strain on emergency services and the overall healthcare system. Experts warn that the lack of coverage can lead to worse health outcomes, increased hospital visits, and higher costs for both individuals and the healthcare system as a whole. As states grapple with the complexities of this transition, advocates are calling for increased funding and support to help streamline the enrollment process and ensure that the most vulnerable populations do not fall through the cracks. The success of these initiatives will be crucial in determining whether low-income Americans can maintain access to the healthcare they need in the coming months.
Poor Americans will face new challenges to enroll, and states will have to build new bureaucracies.