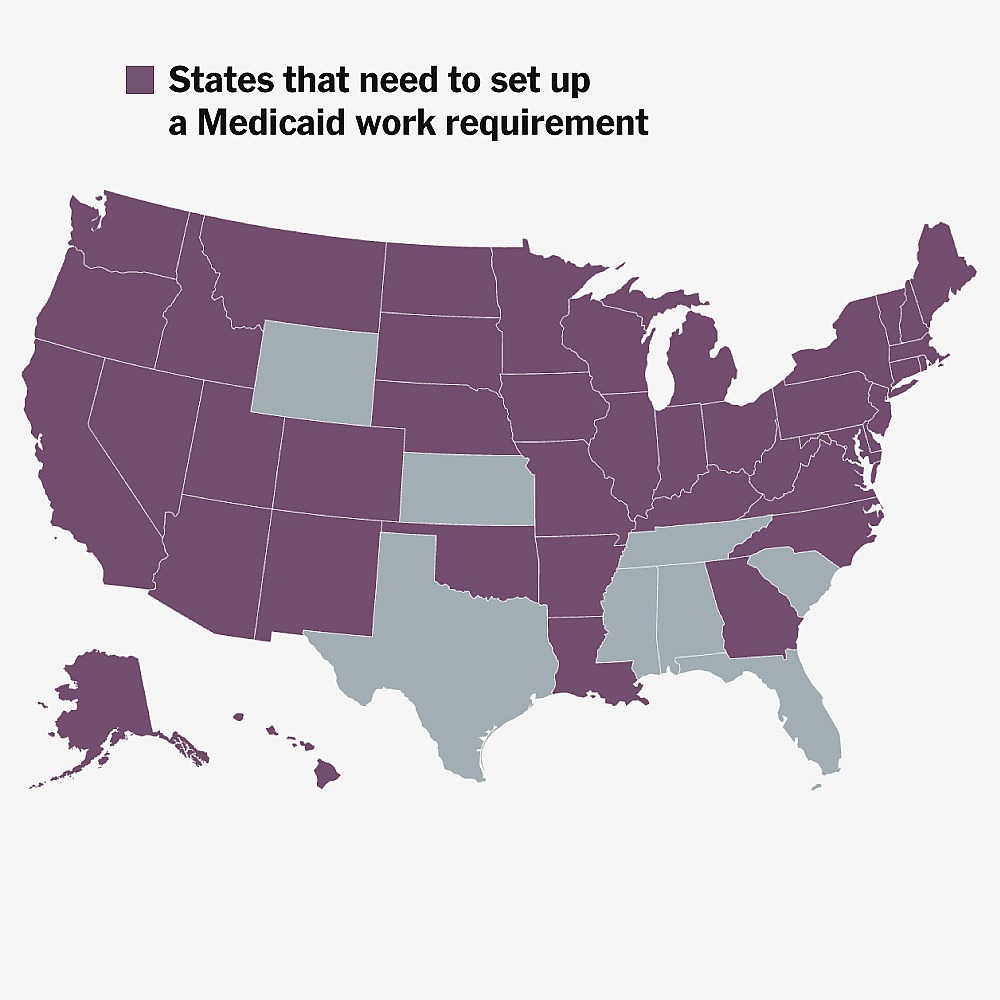
How Medicaid’s New Work Requirement Will Work
In a significant shift affecting low-income Americans, recent policy changes are poised to complicate the enrollment process for health insurance and social services. As states grapple with these new regulations, many are expected to develop additional bureaucratic systems to manage the increased complexity of enrollment. This transition comes in the wake of the expiration of enhanced benefits initiated during the COVID-19 pandemic, which had temporarily expanded access to Medicaid and the Children’s Health Insurance Program (CHIP). With these measures rolling back, millions of Americans are at risk of losing their coverage, highlighting the urgent need for streamlined processes and comprehensive support systems.
The implications of these changes are profound. For instance, states must now navigate the intricate task of verifying eligibility for Medicaid and CHIP, which can be a daunting process for low-income families already facing numerous barriers. In states like Texas and Florida, where the populations of uninsured individuals are already high, the challenge is particularly acute. These states will need to establish new administrative frameworks to handle the influx of applications and ensure that vulnerable populations do not fall through the cracks. Moreover, the shift is likely to exacerbate existing disparities in healthcare access, as those with fewer resources may struggle to complete the necessary paperwork or meet the new requirements.
Examples of potential hurdles include the need for regular income verification and the ability to provide documentation that some families may not have readily available. This bureaucratic burden could lead to increased frustration and confusion among applicants, potentially resulting in significant numbers of eligible individuals remaining uninsured. As states prepare for this transition, advocacy groups are calling for proactive measures to ensure that low-income families receive the assistance they need. This includes outreach programs to educate families about the new requirements and support in navigating the application process. Ultimately, the success of these initiatives will depend on how effectively states can balance the need for oversight with the imperative to facilitate access to critical health services for some of the nation’s most vulnerable populations.
Poor Americans will face new challenges to enroll, and states will have to build new bureaucracies.