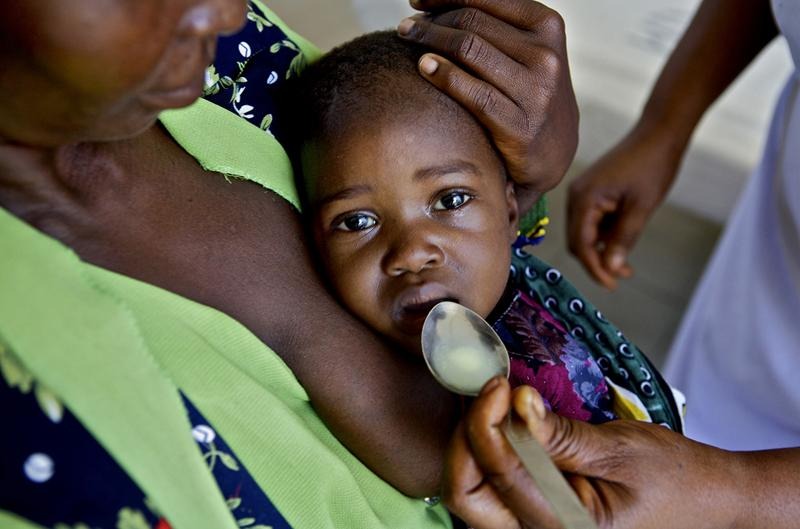
‘A sigh of relief’: New malaria drug succeeds in large clinical trial
In the ongoing battle against antibiotic resistance, the medical community is faced with a critical development: a new class of antibiotics has emerged as a potential game-changer. As traditional antibiotics lose their efficacy due to the rapid evolution of resistant bacteria, this new drug offers a glimmer of hope for treating infections that were previously deemed untreatable. However, the introduction of this powerful medication brings with it a host of ethical and logistical challenges regarding its use, as healthcare providers must navigate the fine line between effective treatment and the risk of exacerbating resistance further.
The new antibiotic, which has shown promising results in clinical trials, targets bacteria that have developed resistance to existing treatments. For instance, infections caused by multi-drug resistant strains of bacteria, such as Methicillin-resistant Staphylococcus aureus (MRSA) and Carbapenem-resistant Enterobacteriaceae (CRE), pose significant threats to patient health and public safety. With the World Health Organization (WHO) warning that antibiotic resistance could lead to 10 million deaths annually by 2050 if left unchecked, the urgency for effective solutions has never been greater. However, experts caution that the emergence of new antibiotics must be managed judiciously. Overuse or misuse of these drugs could accelerate the development of resistance, undermining their long-term effectiveness.
Healthcare systems around the world now face the daunting task of establishing guidelines for the responsible use of this new antibiotic. Decisions must be made about who should receive the drug, when it should be administered, and how to monitor its effectiveness while minimizing the risk of resistance. Additionally, the economic implications of introducing a new drug into the market—especially in low-resource settings—must be considered, as access could be limited by cost and availability. Ultimately, the challenge lies not only in harnessing the potential of this new antibiotic but also in ensuring that it benefits patients without compromising future treatment options. As the medical community weighs these choices, the hope remains that this breakthrough can be part of a broader strategy to combat antibiotic resistance and safeguard public health.
As existing drugs falter because of resistance, the world gets a backup—but hard choices loom on how to use it