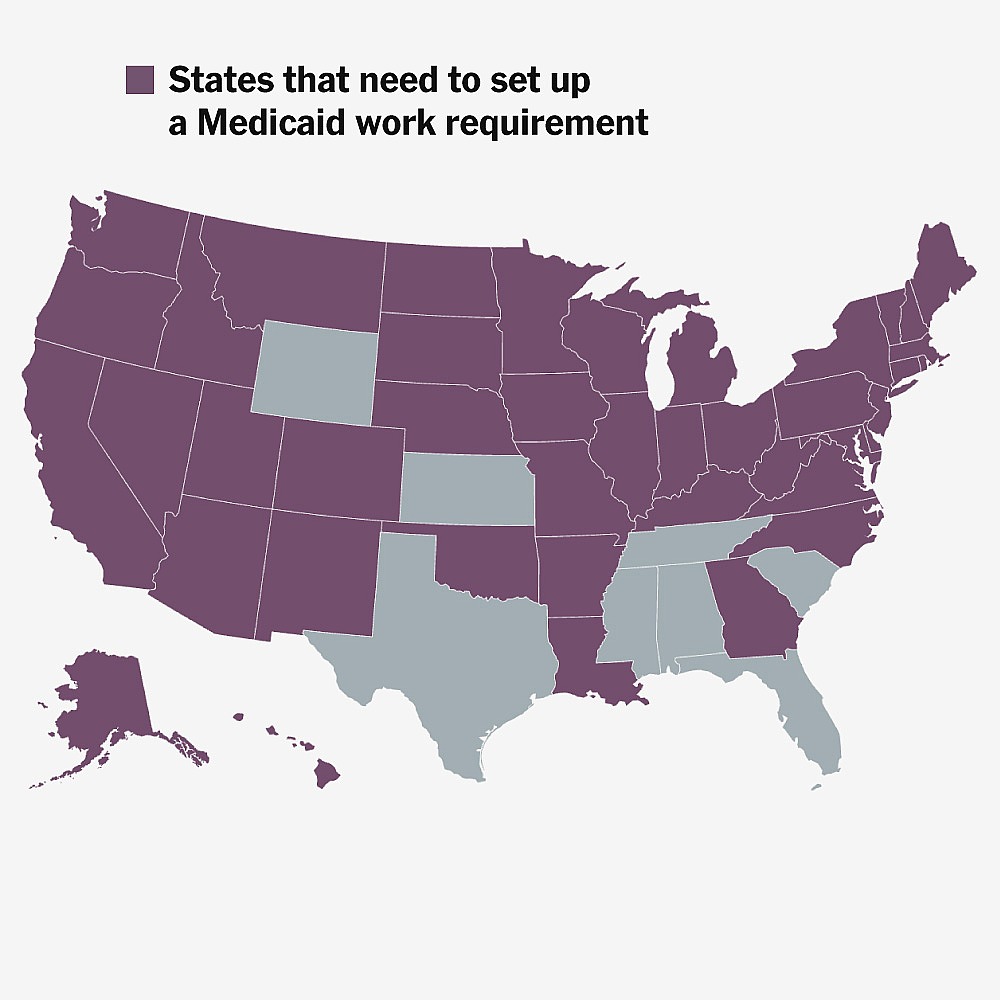
How Medicaid’s New Work Requirement Will Work
In recent developments surrounding healthcare enrollment, low-income Americans are bracing for new hurdles as states prepare to implement changes to their Medicaid programs. The shift comes as a result of the expiration of the COVID-19 public health emergency, which previously allowed for continuous enrollment in Medicaid, preventing many from losing coverage despite fluctuations in income. As states begin to re-evaluate eligibility, millions of individuals could find themselves at risk of losing their health insurance. A report from the Kaiser Family Foundation estimates that approximately 15 million people could be affected, with many facing complex bureaucratic processes to maintain their coverage.
States are now tasked with building new administrative infrastructures to manage the influx of re-enrollment requests and eligibility checks. This is a significant undertaking, as many state agencies have already been stretched thin due to the pandemic and ongoing economic challenges. For instance, states like Texas and Florida, which have historically had higher rates of uninsured individuals, will need to ramp up their outreach efforts and streamline processes to assist those who may be unaware of their need to reapply or who may struggle with the application process. These bureaucratic changes could lead to delays and confusion, potentially leaving vulnerable populations without necessary healthcare services.
Moreover, the transition is expected to disproportionately impact marginalized communities, including people of color and those living in rural areas, who may already face barriers to accessing healthcare. The complexities of navigating the new enrollment processes, combined with the potential for increased administrative errors, raise concerns about health equity. As states move forward, the emphasis will need to be on creating accessible systems that prioritize the needs of low-income families, ensuring that they can secure the healthcare coverage they desperately need. This situation highlights the ongoing challenges within the U.S. healthcare system, where the intersection of policy changes and socio-economic factors can significantly affect access to essential services for the most vulnerable populations.
Poor Americans will face new challenges to enroll, and states will have to build new bureaucracies.