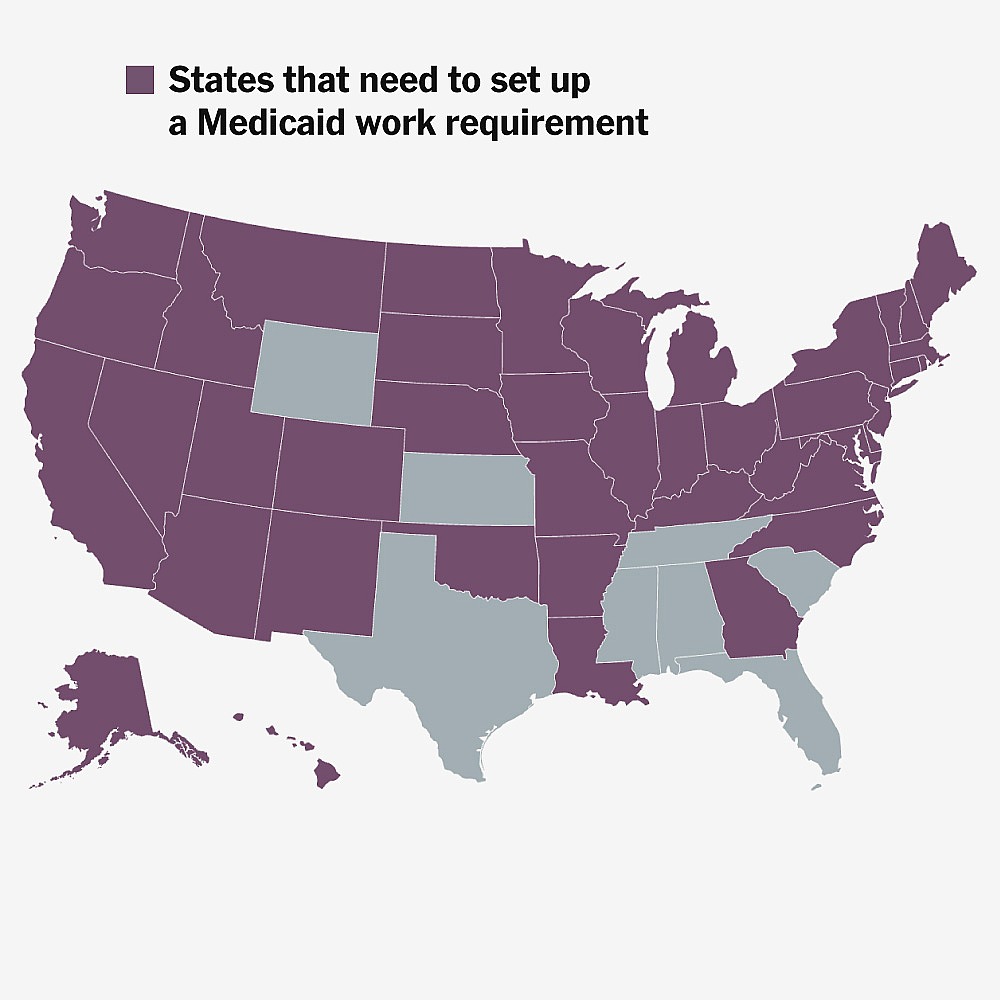
How Medicaid’s New Work Requirement Will Work
In a significant shift in the landscape of healthcare access, the recent changes to Medicaid enrollment processes are set to pose new challenges for low-income Americans. As pandemic-related protections are rolled back, many individuals who previously benefited from continuous coverage will now face the prospect of re-enrollment under stricter guidelines. This transition is particularly concerning as millions of Americans, who may not be aware of the new requirements or lack the resources to navigate the bureaucratic complexities, risk losing their health insurance. The changes come in the wake of the COVID-19 pandemic, which had temporarily expanded access to Medicaid and other health services, allowing many vulnerable populations to maintain their coverage without interruption.
States are now tasked with the daunting responsibility of establishing new bureaucratic systems to accommodate the influx of re-enrollment applications. This involves not only processing renewals but also ensuring that individuals who are eligible for Medicaid are properly informed and supported throughout the application process. For instance, states like Texas and Florida, which have historically faced challenges in efficiently administering Medicaid programs, may struggle to meet the increased demand for assistance. The potential for administrative bottlenecks could exacerbate existing disparities in healthcare access, particularly for marginalized communities that already face barriers to obtaining necessary services. Moreover, the burden of navigating these new systems may disproportionately affect those without internet access or those who are not tech-savvy, further complicating the enrollment process.
As the landscape of Medicaid enrollment evolves, advocacy groups are raising alarms about the potential fallout for millions of Americans who could find themselves uninsured due to these new hurdles. They emphasize the importance of proactive outreach and education to ensure that eligible individuals are aware of their options and understand how to navigate the re-enrollment process. Policymakers are urged to consider the implications of these changes and to implement measures that can streamline the enrollment process, reduce bureaucratic red tape, and ultimately safeguard access to healthcare for the most vulnerable populations. The stakes are high, and the coming months will be critical in determining whether low-income Americans can maintain their health coverage amid these sweeping changes.
Poor Americans will face new challenges to enroll, and states will have to build new bureaucracies.