HIV knows no borders, and the Trump administration’s new strategy leave Americans vulnerable – an HIV-prevention expert explains
The global fight against HIV has faced significant challenges, particularly in the wake of changes implemented during the Trump administration. The recent America First Global Health Strategy, announced by the U.S. Department of State in September 2025, aims to bolster American safety and prosperity by encouraging foreign governments to take greater responsibility for their citizens’ health. Central to this strategy is a commitment to distribute lenacapavir, a breakthrough HIV preventive drug, to up to 2 million individuals in ten heavily affected countries, focusing primarily on pregnant and breastfeeding women. However, critics argue that this approach fails to address the needs of the most vulnerable populations, as it comes alongside severe cuts to the President’s Emergency Plan for AIDS Relief (PEPFAR), which has historically provided crucial funding and support for HIV prevention and treatment globally.
PEPFAR, initiated in 2003, has been instrumental in saving millions of lives and reducing HIV-related deaths significantly over the years. In 2024 alone, the U.S. contributed over 70% of global donor funding to combat HIV, highlighting the importance of American support in the fight against this epidemic. Yet, the Trump administration’s funding pause led to the closure of numerous PEPFAR-supported clinics and outreach programs, disrupting treatment for more than 20 million individuals worldwide. This disruption is expected to result in 4.1 million additional deaths and 7.5 million new infections by 2030. The strategy’s narrow focus on preventing mother-to-child transmission overlooks the critical needs of key populations—such as sex workers, men who have sex with men, and people who use injectable drugs—who are disproportionately affected by HIV but face significant barriers to accessing care due to stigma and discrimination.
Moreover, the shift in funding towards faith-based organizations raises concerns, as many individuals from vulnerable communities report distrust and fear of mistreatment within these settings. Effective HIV care requires not only medications but also tailored approaches that address the unique social and behavioral needs of different populations. The interconnectedness of global health means that neglecting the HIV epidemic abroad ultimately jeopardizes public health and safety in the United States. As the article underscores, a healthy world contributes to a prosperous and secure America, making it imperative to ensure that all individuals, regardless of their circumstances, receive the care and support they need to combat HIV effectively.
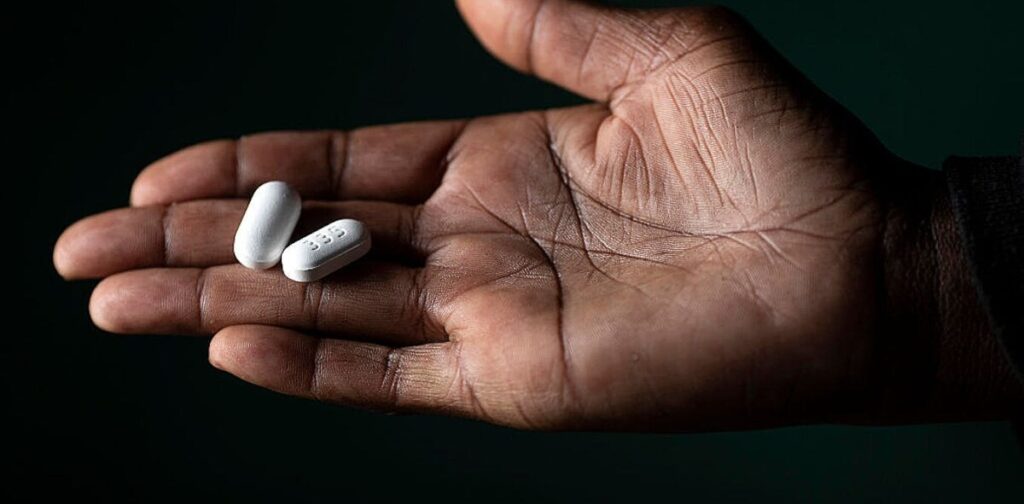
Providing supplies of HIV medications does not ensure they will get into the hands of those who need them most.
Per-Anders Pettersson/Getty Images
Protecting public health abroad benefits Americans.
In a globalized world, diseases and their social and economic impacts
do not stay within national boundaries
. Increased rates of untreated HIV in any part of the world increase the risk of transmission for U.S. citizens.
Changes made in the first year of President Donald Trump’s second term to address the global HIV epidemic, however, may not keep Americans safe.
In September 2025, the U.S. Department of State announced its
America First Global Health Strategy
, a plan that aims to make “America safer, stronger, and more prosperous” by encouraging other governments to take responsibility for their citizens’ health and to promote U.S. commercial and faith-based interests. It
includes the commitment
to purchase and distribute the breakthrough
HIV preventive drug lenacapavir
for up to 2 million people – principally pregnant and breastfeeding women – in 10 countries heavily affected by HIV.
However, the plan does not ensure the most vulnerable will be able to access HIV care. It comes on top of
eliminating billions of dollars
of U.S. financial support to global health programs. And it undermines
one of the most effective
foreign assistance programs in U.S. history, the
U.S. President’s Emergency Plan for AIDS Relief, or PEPFAR
.
I have spent four decades
evaluating HIV programs
and have
studied barriers to HIV prevention and care
in the U.S. and in other countries. The Trump administration’s strategy not only reverses decades of progress toward
international targets to end AIDS by 2030
, I believe it also puts Americans at risk.
Disrupting PEPFAR caused global harm
In 2024, the U.S. supplied
over 70% of donor government funding
to end the HIV epidemic globally. Much of this aid was through the
President’s Emergency Plan for AIDS Relief
, a suite of programs designed to expand access to prevention, testing and treatment.
Since President George Bush initiated the program in 2003, PEPFAR has saved an
estimated 26 million lives
.
HIV deaths have declined by 70%
since 2004, and new infections fell after the program’s inception. PEPFAR helped
put the world on track
to ending the HIV pandemic by promoting access to highly effective drugs, supporting community-led outreach and programs, and building health care infrastructure.
HIV clinics dependent on PEPFAR funding have shuttered with the Trump administration’s significant cuts to the program.
AFP/Getty Images
On Jan. 20, 2025, President Donald Trump signed an
executive order
that paused funding for all foreign aid programs,
including PEPFAR
. It shuttered PEPFAR-supported clinics and outreach programs, halted medical and supply shipments, and prompted mass layoffs of the global HIV workforce. It also dissolved USAID, which
provided essential infrastructure for PEPFAR
to do its work.
The Trump administration’s foreign aid pause disrupted access to HIV treatment for
more than 20 million people
worldwide and access to prevention for millions more. These actions are projected to cause
4.1 million additional deaths and 7.5 million new HIV infections by 2030
.
The full
extent of the damage
will become
increasingly clear
with time.
Destabilizing HIV prevention and care
Legal pushback
in the months following the Trump administration’s dismantling of USAID allowed limited parts of PEPFAR to restart. However, access to HIV medication was
explicitly limited to only pregnant and breastfeeding women
. This strategy excludes prevention and care to the majority of people who are vulnerable to HIV infection.
The Trump administration’s new global HIV prevention strategy prioritizes
preventing mother-to-child HIV transmission
. About
120,000 children
under the age of 5 were newly infected with HIV in 2024, or around 9% of the 1.3 million new infections that year.
However,
55% of new infections worldwide occur among “key populations
,” a catchall term coined by UNAIDS and WHO. These include sex workers, people who use injectable drugs, men who have sex with men, transgender people, prisoners, and the sex partners of these individuals. These groups are considered “key” because of their heightened vulnerability to HIV infection and because ending the HIV pandemic cannot be achieved without their access to prevention, testing and treatment.
Stigma and discrimination
,
human rights abuses
,
criminalization
and
underfinancing
of programs specific to these people’s needs are
significant barriers to their care
.
Loss of peer-to-peer support
In countries with
legal and social environments
that discourage vulnerable people from seeking HIV services,
trusted and knowledgeable peers
can be a lifeline.
PEPFAR used to fund services
designed and implemented by the peers
of vulnerable people. People from vulnerable communities were
directly involved in
ensuring their peers had access
to appropriate HIV services and remained in care. They also directly shaped their countries’ national HIV plans.
Meeting vulnerable communities where they are is critical to effective HIV care.
STR/AFP via Getty Images
The Trump administration’s new strategy favors pregnant and breastfeeding women and cuts out other vulnerable communities. It proposes
funding government health care workers
in lieu of peers without ensuring these workers will be adequately equipped to provide unprejudiced care. The plan
withdraws support for community-led, nongovernmental organizations
that bridge gaps in care and offer sensitivity training to providers.
Many people who are vulnerable to or living with HIV view government-run medical care with
profound distrust and apprehension
. Some participants in my own research have told me they would
rather die than seek care in a government-run facility
. They recount dehumanizing experiences in these facilities, including undergoing invasive procedures without consent and being openly humiliated. Health care workers have also
violated patient confidentiality
by disclosing patients’ sexuality and HIV status to family members, friends, neighbors, landlords or employers.
Fear of repercussions
– arrest, violence, loss of housing and employment, and blackmail – further heighten fear of health care settings. Research has shown that many people living with HIV from vulnerable populations report
encountering these forms of discrimination and stigma
when seeking health care. Even more
report being hesitant to seek care
.
Faith-based organizations
The strategy
shifts funds to faith-based institutions
, citing potential financial support from tithes and donations as well as greater reach through faith leaders. However, research has shown that faith-based and government health care institutions evoke fear of
stigmatization
,
mistreatment
,
arrest
and
denial of services
among many who are most at-risk for HIV.
Conservative evangelical groups such as Family Watch International – a
designated hate group
by the Southern Poverty Law Center – have authored some of the world’s most
punitive anti-homosexuality laws
in countries such as Uganda, where HIV remains inadequately controlled. They also advocate for the
scientifically debunked practice of conversion therapy
and are
leading actors
in global movements against LGBTQ+ human rights,
comprehensive sexuality education
and reproductive health services.
HIV requires a unique response
Effectively addressing HIV requires more than providing supplies or medical treatment. Although
treatments to manage
and
prevent HIV infection
are highly effective under ideal conditions, these are not the circumstances of many people living with and vulnerable to HIV. Treatment is lifelong and needs to be taken regularly. Additionally, the epidemic is often concentrated in networks of people who face societal discrimination, making care retention and engagement difficult.
The Trump administration’s
new global health strategy
requires community health care workers to consolidate their work across four distinct diseases: malaria, polio, tuberculosis and HIV. However, very different populations are vulnerable to these diseases, and each has unique social, psychological and medical concerns and needs.
Cuts to PEPFAR have led to thousands of deaths.
AP Photo/Mark Schiefelbein
For example,
malaria
and
polio
primarily affect children under 5, but the former requires strategies to reduce the mosquito bites that transmit disease, while the latter requires childhood immunization. Meanwhile, HIV primarily
affects adolescents and adults
and requires interventions addressing sexual health and harm reduction.
Research and lessons learned over decades of global health work suggest that
carefully tailoring prevention and care strategies
to each vulnerable population and addressing their unique social, behavioral, structural and medical needs improves their effectiveness.
A healthy world makes a safe and prosperous US
The
55 countries
that most recently benefited from PEPFAR may seem far from U.S. soil. But in an interconnected world, their epidemic is an American epidemic.
The Trump administration’s reversal of decades of progress on ending the HIV pandemic – and weakening U.S. leadership and humanitarian effort in the fight against HIV – has
already led to thousands of deaths
. Every new HIV infection will incur
global economic and societal costs
by draining labor capacity in high-burden countries while increasing health care and caregiving costs. This global insecurity and economic instability has precedents in the
initial HIV crisis
and the
COVID-19 pandemic
.
Ensuring people living with HIV worldwide receive appropriate treatment and care
advances U.S. national security, diplomatic and economic interests
. Ensuring that citizens in other countries enjoy good health permits their economies to thrive and
America’s in turn
. I believe a healthy world is a more prosperous, peaceful and stable world, to everyone’s benefit.
Robin Lin Miller has previously received research and evaluation funding from the U.S. Department of State, Centers for Disease Control and Prevention, National Institute of Mental Health, National Institute of Drug Abuse, the Eunice Kennedy Shriver National Institute of Child Health and Development, American Foundation for AIDS Research, Michigan Department of Community Health, Michigan AIDS Fund, AIDS Foundation of Chicago, and the Health Services Improvement Fund.